What Your Liver Tests Are Really Telling You About Your Weight
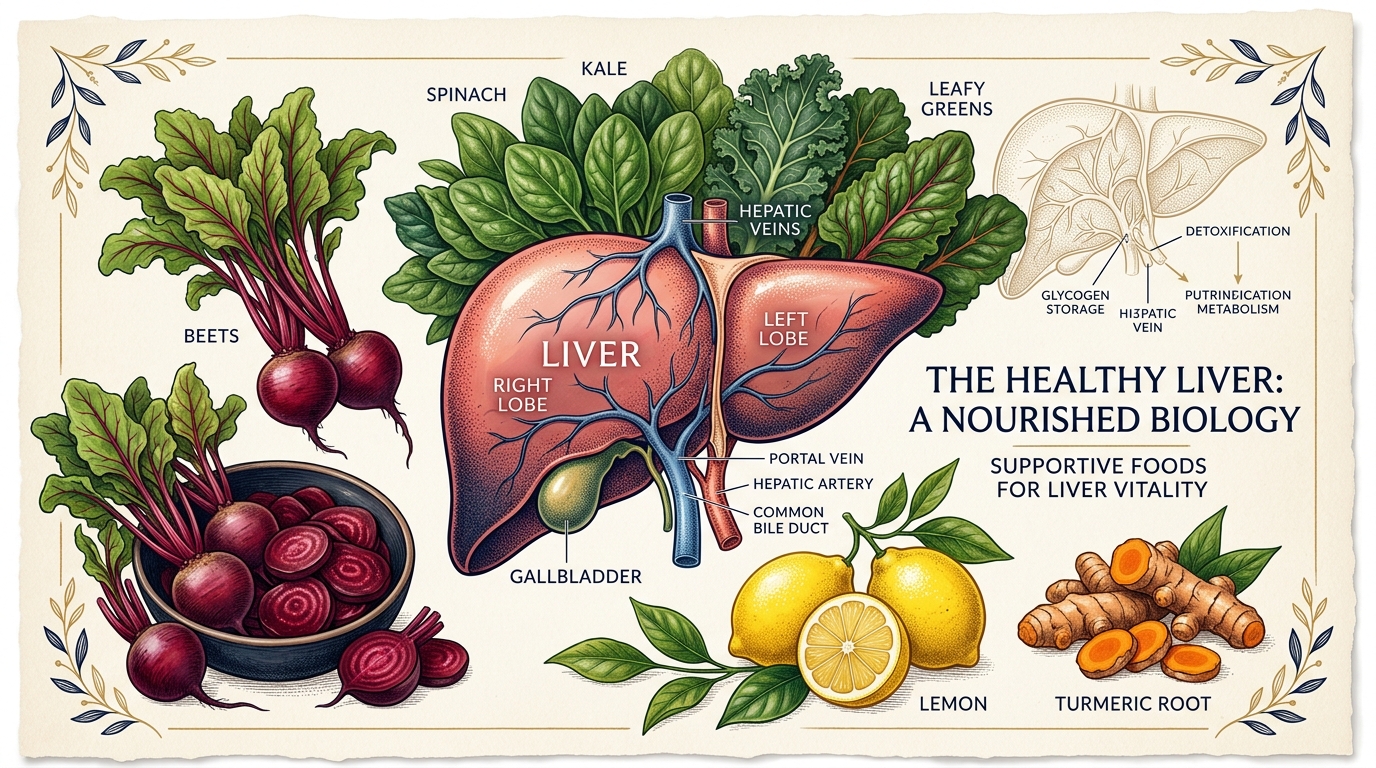
What Your Liver Tests Are Really Telling You About Your Weight
You get your annual bloodwork back. Everything looks "normal." Your doctor says you're fine. And yet—you're still gaining weight, you're tired, your clothes don't fit, and you can't seem to lose even five pounds.
This is the moment to ask a deeper question: What are your liver tests really telling you?
Your liver is not just an organ that filters toxins. It's your metabolic headquarters. It's the command center for blood sugar, fat metabolism, and hormone breakdown. When your liver is overwhelmed—and most perimenopausal women's livers are—weight loss doesn't happen. No matter how disciplined you are.
The signal comes through your liver tests. And if you know how to read them, they'll tell you everything.
The Liver's Real Job
Your liver does three things that matter for weight loss:
-
Processes insulin and glucose. When you eat carbohydrates, your liver captures glucose and stores it as glycogen (or converts excess to fat if glycogen stores are full). If your liver is overwhelmed by constant carbohydrate load, it can't manage this job well.
-
Manufactures and packages fat for energy. Your liver makes ketone bodies when fat is available. It also synthesizes VLDL (very low-density lipoprotein)—the cholesterol particle that carries fat through the bloodstream. If your liver is dysfunctional, this process falters.
-
Clears hormones and metabolic waste. Your liver breaks down estrogen, progesterone, and other hormones. It processes metabolites. If it's congested, hormonal backup occurs—and excess estrogen recirculates, which drives weight gain and bloating.
When your liver is working well, your metabolic signal is clean. Insulin gets managed, fat gets burned, hormones clear. When it's not, everything backs up.
What Fatty Liver Actually Means
Non-alcoholic fatty liver disease (NAFLD) now affects roughly 25-30% of women. Many have no symptoms. Many have normal liver enzyme tests.
Here's what's happening: fat is accumulating inside liver cells. The liver becomes inflamed. Its ability to process glucose and manage insulin declines. But the classic liver enzymes—ALT (alanine aminotransferase) and AST (aspartate aminotransferase)—might still be in the "normal" range.
Why? Because those enzymes only elevate when liver cells are actively dying. Mild to moderate fatty liver can exist silently.
This is critical: Normal liver enzymes do not equal a healthy liver.
Reading Your Liver Tests
If your lab report shows:
ALT elevated (above 40 IU/L): This is the most sensitive marker for fatty liver. ALT lives inside liver cells. When those cells are stressed or damaged, ALT leaks into the bloodstream. If your ALT is elevated, your liver is signaling distress.
AST elevated: Less specific than ALT, but when both are elevated, it points to liver inflammation.
AST/ALT ratio high (above 1.0): When AST > ALT, it can signal more advanced fibrosis. Your doctor should be taking this seriously.
GGT elevated (above 55 U/L): Gamma-glutamyl transferase. Elevated GGT points to oxidative stress and insulin resistance. It's one of the best predictors of metabolic dysfunction.
Bilirubin elevated: Suggests the liver isn't processing bile well. Metabolic dysfunction is progressing.
Albumin low (below 3.5 g/dL): Albumin is made in the liver. Low albumin means reduced liver synthetic capacity—the liver is losing function.
But your ALT is normal... And yet you have every sign of metabolic dysfunction—weight gain, fatigue, brain fog, hormone disruption. This is the silent fatty liver picture. Your liver is congested but not yet inflamed enough to elevate enzymes.
Why This Matters for Your Weight
Here's the link: Fatty liver = insulin resistance.
When your liver accumulates fat, it becomes less responsive to insulin. Insulin can't do its job—which means glucose doesn't clear from the bloodstream as efficiently. Your pancreas keeps releasing more insulin. Higher insulin tells your body: Store fat. Don't burn it.
Meanwhile, your liver can't manufacture ketone bodies effectively (because it's clogged). You can't access fat as fuel efficiently. You're stuck: unable to burn fat, driven to store fat, exhausted by the metabolic struggle.
This is why women with fatty liver struggle with weight loss even when they're eating well. The problem isn't willpower or calories. It's a metabolic signal problem.
What Metabolic Repair Means for Your Liver
When you shift your macros to 70/20/10—high fat, adequate protein, minimal carbs—you're sending a new signal to your liver:
Stop processing constant glucose. Start making ketones. Start mobilizing stored fat.
Over time: - Glycogen stores replete (the glucose chaos settles) - Insulin drops (the store-fat signal quiets) - Ketone production increases (your liver gets back to manufacturing fuel) - Hepatic fat content decreases (your liver stops accumulating fat) - Inflammation recedes
Your liver starts working again.
And this is where it gets powerful: as your liver recovers, your metabolic signal cleans up. Insulin resistance improves. Fat loss becomes possible. Fatigue lifts. Brain fog clears.
You're not fighting your body anymore. Your body is working with you.
The Electrolyte Piece
One more detail: your liver needs electrolyte support for this transition. Sodium, magnesium, and potassium are cofactors in metabolism. When you shift to lower carbs, you lose water and electrolytes quickly. A depleted liver can't perform at peak.
This is why the metabolic approach includes: - Celtic or Himalayan salt (real salt, mineral-rich) in every meal - Magnesium glycinate 200-400mg daily (supports energy metabolism and liver detoxification) - Potassium from leafy greens and low-carb vegetables
These aren't supplements. They're structural support for the metabolic repair happening in your liver.
What You Can Do Right Now
-
Get your liver tests run. Ask for ALT, AST, GGT, ALP, bilirubin, albumin. Get the ratios. If you have a recent panel, ask to see the numbers (not just "normal").
-
Track your waist circumference. Waist-to-height ratio is a better predictor of fatty liver than BMI. Visceral fat (belly fat) is what accumulates around your liver. Waist size often shrinks before scale weight shifts—especially if your liver is repairing.
-
Reduce the carbohydrate load. Not forever, but therapeutic carb reduction (net carbs under 25g daily) gives your liver a break from constant glucose processing. Your liver can begin to heal.
-
Add salt and magnesium. Not excess, but adequate electrolytes support metabolic function at every level.
-
Retest in 8-12 weeks. If you're managing metabolic dysfunction well, your ALT should drop, your GGT should normalize, and you'll feel the shift.
One More Thing
If your doctor dismissed your concerns because your liver "looks normal," I want you to know: trust your body. If you feel metabolically broken, something is likely dysfunctional even if the standard markers don't reflect it yet. The metabolic approach addresses the root cause—the signal problem—not just the numbers on a lab report.
Your liver is smart. Give it clean signal (low insulin). Give it support (electrolytes). Give it time. It will repair.
Ready to understand the full metabolic picture? I invite you to join the free 5-Day Metabolic Challenge, where we walk through the science of your liver, your metabolism, and how these connect to your weight and energy. You'll get a day dedicated to lab interpretation and what your body is actually trying to tell you.
[Join the Free 5-Day Metabolic Challenge]
Your liver is part of your weight story. Let's make sure you're reading it correctly.
Latest Articles
Quick reads for steadier days.